Current gene-editing uses

New gene-editing technologies are enabling a broad range of applications from basic biological research to biotechnology and medicine (see FIG. 2). Learn more about how these these new technologies are being used and applied.

Medical applications in treatments and research
Of the approximately 25,000 identified genes in the human genome so far, mutations in over 3,000 have been linked to disease. Gene-editing tools are now being used to understand how gene variants are linked to disease in mammalian cells and whole animal models, indicating the potential for this technology to be used to understand and treat human disease (see FIG. 3).
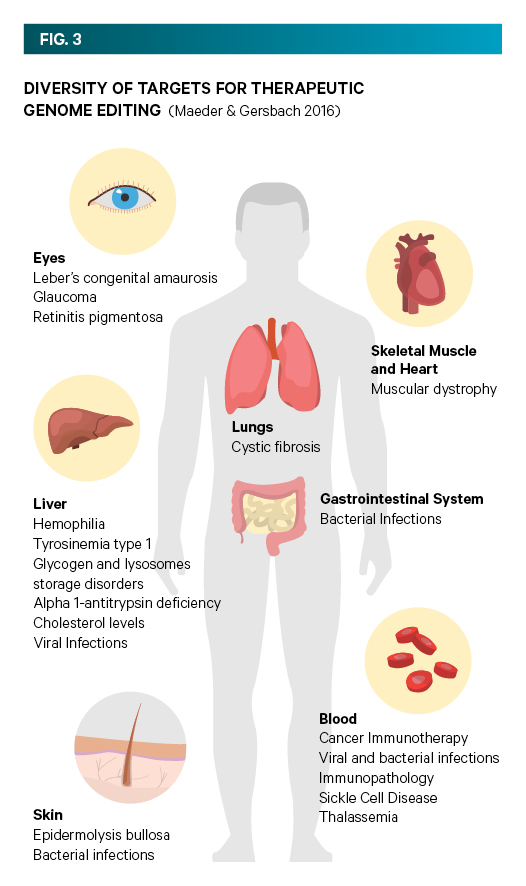
For example, CRISPR has been used in research mouse models to correct a mutation in genes responsible for Hepatitis B, haemophilia, severe combined immunodeficiency, cataracts, cystic fibrosis, hereditary tyrosinemia and inherited Duchenne muscular dystrophy.
Clinical trials with patients are underway in the US using ZFN to modify the genes of immune-system cells to treat HIV. HIV infects and destroys immune system cells and key genes within these cells have been modified using ZFN to make them resistant to HIV, and the cells then transplanted back into patients.
The Great Ormond Street Hospital in the UK has used TALENs for gene editing in donated blood cells to disable the gene which the immune system uses to recognise ‘foreign’ cells. This allowed a patient to receive donated blood cells, without the donor cells attacking the patients’ healthy cells. In June 2016, a federal biosafety and ethics panel in the US approved a clinical study in patients using CRISPR-based genome-editing to create genetically altered immune cells to attack three kinds of cancer.
Gene editing is also being used by researchers to try to overcome allergic reactions to chicken eggs, which prevents about 2% of children worldwide from receiving many routine vaccinations. Researchers at Deakin University in Australia are working with gene modifications using CRISPR to produce hypoallergenic eggs.
The use of gene-editing technologies in the early stage embryo allows modifications which can be passed on to future generations. In the UK, the Human Fertilisation and Embryology Authority (HFEA) has approved an application for the use of CRISPR in healthy human embryos to help researchers to investigate the genes involved in early embryo development. This could lead to improvements in assisted reproductive technologies used to treat infertility, although the CRISPR technology itself will not form the basis of a therapy. In China, researchers have used CRISPR in non-viable human embryos to genetically modify genes responsible for ß-thalassemia, a potentially fatal blood disorder, and to modify genes in immune cells to develop increased HIV resistance.
Agricultural applications
In agriculture, the new gene-editing technologies make it possible to modify a range of agriculturally-important organisms easily, cheaply, and if desired, without introducing foreign DNA sequences.
Food production
In the US, researchers have used gene-editing technologies on agricultural crops such as maize, soybean, sorghum, and developed a rice resistant to bacterial blight. In commercial development, the common white button mushroom has been modified by CRISPR at Penn State University to prevent them from becoming off-colour by targeting a gene that produces an enzyme that causes browning. Further, DuPont Pioneer have used CRISPR to produce a higher-yielding waxy corn variety and Calyxt Plant Sciences Inc. have produced soybean lines that are low in polyunsaturated fats, using TALENs.
Chinese researchers have similarly used TALENs and CRISPR to modify a range of agriculturally important plants and animals, including maize, rice, and wheat. They have also used the techniques to develop goats with longer coats (for Angora) and more muscle (for increased meat yield). Elsewhere in the world, researchers have used the techniques to modify barley (Denmark); wheat (India); and to study allergenic milk protein production in cow embryos cultured in the laboratory (New Zealand).
Animal health and welfare
In the US, hornless dairy cattle have been produced using gene editing to avoid the need for painful de-horning and to prevent animals injuring each other during transport. Using TALENs, the genetic code that makes dairy cattle have horns has been substituted for the one that makes Angus beef cattle have none. The University of Missouri has also bred the first pigs resistant to Porcine Reproductive and Respiratory Syndrome by suppressing the production of a protein within the pigs that the virus uses to help it spread.
African swine fever is a highly contagious disease that kills up to two-thirds of infected animals. In Scotland, ZFN has been used by the University of Edinburgh to modify a gene in pigs to the version of the gene found in warthogs, to produce pigs that are potentially resilient to the disease. The university has also used gene editing to modify chicken genes so they don’t spread bird flu by introducing a gene that produces a ‘decoy’ molecule that interrupts the replication cycle of the bird flu virus, thereby restricting its transmission.
In China, TALENs have been used to add a gene that is found in mice into cattle to improve tuberculosis (TB)- resistance. The modified cattle have immune cells that are better at slowing the growth of the disease and are less susceptible to developing the internal symptoms of TB.
Pets
In China, CRISPR has been used to create micro-pigs which are approximately half the size of their non-modified counterparts, which can be sold as pets.
Biocompound production
By using gene-editing technology to manipulate biological pathways, new materials are being developed, such as algae-derived porous silica-based particles for drug delivery, CRISPR modified silkworms to produce spider silk, algae-derived lipids for biofuels, and microbial production of pharmaceuticals and commodity chemicals such as ß-carotene, L-lysine, and mevalonate.
Environmental applications
Gene-editing tools have not been used to date in the conservation of wildlife, but their use in the control of non-native invasive organisms is being explored with the use of gene drives.
Gene drives
In 2015, researchers demonstrated the use of CRISPR to develop ‘gene drives’, a genetic system named for the ability to ‘drive’ themselves and nearby genes through populations of organisms over many generations.
In sexual reproduction, offspring inherit two versions of every gene, one from each parent. Each parent carries two versions of the gene as well, so chance (50:50) normally governs which particular variant of the gene that will be passed on.
But ‘gene drives’ ensure that the genetic modification will almost always be passed on, allowing that variant to spread rapidly through a population (see FIG. 4). So far, ‘gene drives’ have been developed in yeast, the fruit fly, and two mosquito species.
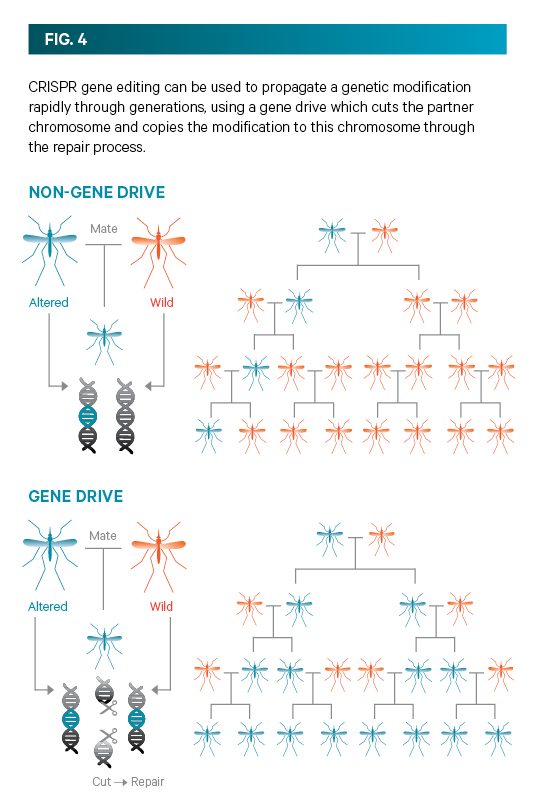
One of the mosquito gene drives, developed in the US by researchers at the University of California, causes a malaria-resistance gene to be passed on to the mosquitoes’ offspring, meaning they are unable to transmit malaria in mice. The other mosquito gene drive strategy, developed by Imperial College in the UK, propagates a gene that sterilizes all female mosquitoes (which could suppress specific mosquito populations to levels that will not support malaria transmission).
Changing research approaches
In biological research, gene editing can increase the speed and ease of creating new animal-based or cellular models for disease, and it is proving to be an important tool in the study of cell development.
Rapid generation of cellular and animal models
Many human illnesses, including heart disease, diabetes, cancer and various neurological conditions, are affected by numerous variants in genes. Working out the impact of these variants on the illness with the help of animal models has been a slow process. To create these animal models, mutations need to be introduced into multiple genes. But using conventional tools to create a mouse with a single mutation can take up to a year and cost US$20,000 to produce. If a scientist wants an animal with multiple mutations, the genetic changes must be made sequentially, and the timeline for one experiment can extend into years. In contrast, CRISPR has allowed the creation of a strain of mice with multiple mutations in a few weeks, with the CRISPR tools costing as little as US$30.
Functional genomic screens
Cultures of cells developed from a single cell, which has a uniform genetic make-up, are used to examine the contribution of genes to biological processes. CRISPR can now be used to rapidly generate thousands of these different cell lines, with each cell line having a different gene switched off, to speed up the search for DNA sequences linked to specific biological processes.
Exploring gene expression
Almost every cell in the human body has roughly the same DNA sequence but cells use their DNA code in different ways, depending on where they are located in the body. One way that genes are controlled is by DNA-packaging proteins called histones. In 2015 it was reported how CRISPR could be used to attach to and switch on these proteins, to determine whether they cause changes to the growth and development of the organism.
Tracing cells during development
In 2016 it was discovered that CRISPR can be used to mark cells whenever they divide based on a specific pattern (or barcode) of deletions and insertions. This technology now allows researchers to re-construct a ‘family tree’ of the cells that compose an animal’s body, revealing which cells spawned others. The use of this technique is now also being considered to record a cell’s history in response to environmental signals, or to trace the evolution of tumours.
